|
She assumed she’d been in a coma for almost a year, until a nurse told her they were only an April Fools prank.Īccording to the Society of Critical Care Medicine, between 30 and 80 percent of ICU survivors struggle with some sort of cognitive impairment after their stay. When she finally came to, the hospital wing was covered in Christmas decorations. Her imagined exploits on the “show” felt real, but everything happening in real life felt like a dream. Mendez says she spent 10 days on the ventilator thinking she was a character in the Netflix show On My Block. The confusion Mendez felt coming off of the ventilator is common for patients with extended ICU stays-so common it has a name: “ICU delirium.” The extreme stress of critical illness on the body, combined with the sedative drugs and the foreign surroundings of the ICU, leave many people feeling confused and disoriented, occasionally plagued by memories of things that never happened. Many of them will require mechanical breathing devices called ventilators to keep them alive. An even smaller percentage will require care in the ICU-often because of a lung condition called acute respiratory distress syndrome (ARDS). Of the hundreds of thousands of Americans projected to contract the coronavirus, a small percentage will require hospitalization. “The question is, how will the system step up to meet this?” “I believe and I feel this with every part of me, that the same way there's been a surge in need for hospital beds, there's going to be a surge in need for rehab beds,” said Miguel Escalón, the vice chair of the rehabilitation department at Mount Sinai. And some are not sure we’re ready for the influx of ICU survivors this crisis will bring. Now physicians say they are witnessing many of these effects in COVID-19 survivors, at a scale they’ve never seen before. An ailment called Post-Intensive Care Syndrome (PICS) causes cognitive, physical, and psychological problems in up to 80 percent of all critical-care survivors. 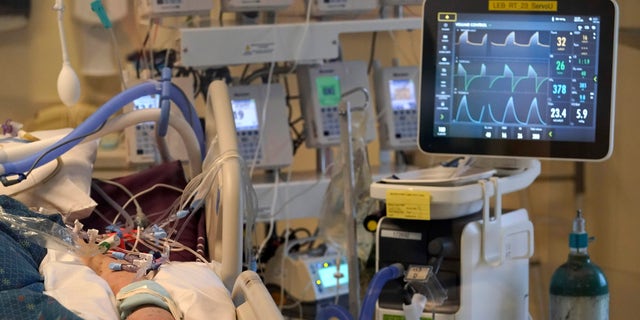
Use alcohol-based hand sanitiser on entry to the health service, after using the lift, handrails etc.Decades of research shows many of the sickest ICU patients will never return to their former selves.Children less than 16 years are permitted for short periods if their visit fits with end of life support for a sibling, parent or grandparent.Visitors from Melbourne or other ‘hot spot’ locations are permitted to visit immediate family nearing end of life if screening requirements are met and they are a nominated.Breathlessness or breathing difficulties.A temperature higher than 37.5 degrees on arrival.Had close contact with someone who has tested positive for COVID-19 or is awaiting test results.Tested positive for COVID-19 or are awaiting results.Arrived / returned from overseas in the last 14 days.In the event that family have travelled and need somewhere to sit in a private space, whilst practicing social distancing, we have made the Malka Room available during the day and at night time.Īll staff and visitors to the health service are required to undertake COVID-19 screening prior to entry to the health service, on every occasion of entry.Īll staff and visitors must provide their name, contact details and reason for visit on every occasion of entry. When not with the patient, we ask families to leave the hospital, if this is a feasible option. We ask families to provide the names and contact numbers of nominated visitors to the Nurse in Charge. We ask families to develop a visiting roster with loved ones, allowing no more than two people to be present with the patient at any given time.  
Where there are greater than two immediate family members who wish to visit, this may be facilitated using a rotational roster. ‘If you are providing care and support at the end of a persons life, where the person is unable to go home from hospital and their condition is deteriorating in a manner where death is likely in the next few days (up to 14), up to two people may visit at any one time with no limits on the number and duration of visits.’ The Victorian Department of Health and Human Services (DHHS) describe visitation restrictions for End of Life Care and Support as We will work with you to establish a visiting routine that best suits your situation. Here at Echuca Regional Health (ERH) we wish to support people who are nearing end of life by supporting their family and friends to visit, whilst continuing to provide a COVID Safe environment for all patients and staff. 
Contact the Nurse Unit Manager during business hours, or the Nurse In Charge out of hours, for further information and individual planning.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
